By Sharon E. Hohler, RN, BSN, CNOR
Behind the double doors of an operating room lives another world. The environment is frigid in temperature and the decor utilitarian. Everything in the OR must able to withstand multiple cleanings daily. No wall decorations are used except maybe a crucifix to remind staff of the organizational heritage and mission.
People work every day behind closed doors inside operating rooms. They wear scrubs, paper hats, and masks. They are the operating room staff and several jobs are represented. A routine general surgery involves a minimum of 5 staff: anesthesia care provider, surgeon and his assistant, circulating nurse and scrub technician. Complicated surgeries involve more staff.
This is the world I entered as a young nurse 40 years ago. I worked every day in the operating room. As the years passed, new technologies evolved and scientific studies changed practices. Evidence based practices became a key phrase meaning best scientific-based practices. While practices changed, one thing never changed: patients undergoing surgery need an advocate.
Nurses act as patient advocates daily around the world. Nowhere is it more needed than the operating room. Years ago I was discussing a patient with his surgeon before he started the procedure and he said to me, “Who do you think you are–a patient advocate?” This struck a cord deep inside and I responded, “Yes sir, that’s exactly what I am. This patient is under general anesthesia and cannot speak for himself.”
Trust.
Nursing is the most trusted profession.
This is according to a 2019 Gallup poll.1 When assessing ethics and honesty, nursing beats out all others including physicians, clergy, teachers and police officers.
Patients in Pre-op Holding Room are almost always anxious. They are afraid of many things in this strange environment. A friendly OR nurse enters the room and washes her hands. (If you wash hands as you walk in, they see that you care about preventing infection).
The nurse introduces herself and starts asking questions, verifying details such as patient identity, birthdate, allergies, etc. The patient’s medical and surgical history, and current medications have been considered in the perioperative nursing care plan.2 The patient at this point begins to trust the OR Nurse to take care of him.
When the OR nurse brings the patient back to the OR room, it’s cold and he needs those warm blankets she placed over him. As he scoots over the OR table, he appreciates that she pre-warmed the bed but he still needs more warm blankets. Anesthesia staff greets the patient and they begin placing EKG monitors over his chest, pulse oximeter probe on his finger and a blood pressure cuff on his arm.
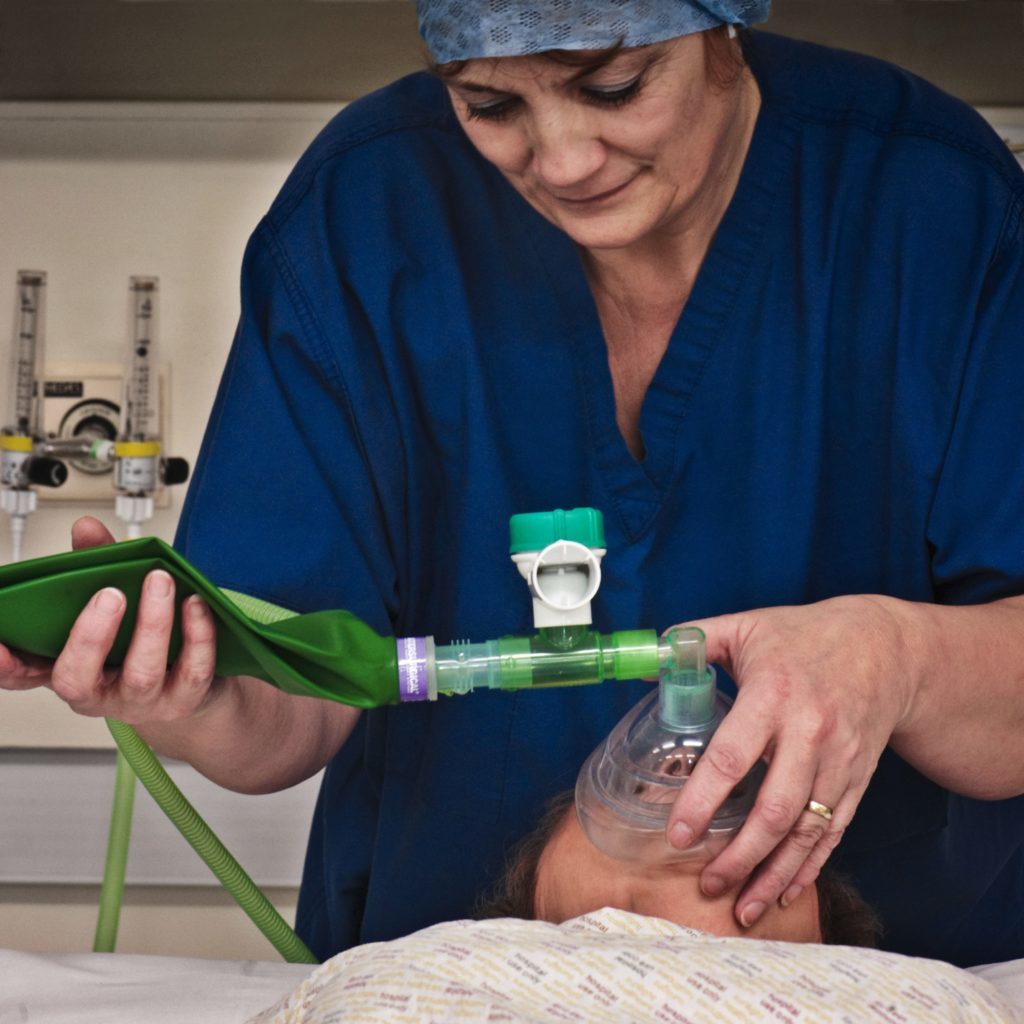
As the anesthesia care provider begins giving the general anesthesia drugs, the patient goes off to sleep. Because of the advocacy provided, he now trusts that these strangers will take care of him.
Some critically important things happen at the beginning of a surgical procedure: getting the patient off to sleep and maintaining airway and critical bodily functions.
The Comprehensive Surgical Checklist from the Association of PeriOperative Nurses includes the “time out” which ensures:2
- That the correct patient is having the correct surgery
- Correct laterality
- All needed implants are available in the OR
- Fire safety protocols are followed
- Appropriate antibiotics given within the correct time frame
- Equipment check for proper function
- Proper sterile technique is utilized during preparation and throughout surgery
- Operative skin prep is applied as recommended
During the procedure, the OR nurse is attentive: she obtains and opens needed supplies and implants. She documents an accurate, clear picture of the surgical experience as the patient sleeps under general anesthesia.
After the surgeon is finished, he leaves to speak to the patient’s family. The anesthesia care provider and the nurse are at the patient’s side while he awakens and is transported to Post Anesthesia Care Unit. The OR nurse and anesthesia care provider give a handoff report to the PACU nurse accepting the patient. This final act of patient advocacy insures that this patient’s pertinent information is received by the PACU nurse and influences the care she gives him. As the OR nurse walks back to the OR room to finish charting and help with cleaning, she knows she has done her job as an OR nurse: patient advocate behind a mask.
Guest Blogger Bio
Sharon E. Hohler, RN, BSN, CNOR, and Clinical Nurse IV, practiced OR nursing at Saint Francis Medical Center in Cape Girardeau, Missouri for 40 years. She retired from full time July 2018, but continues in a per diem role. She is also a multi-published writer with two non-fiction books and 17 peer-reviewed articles published in nursing magazines/journals.
References
1. Norman, J. (2019) Americans Rate Healthcare Providers High on Honesty, Ethics. Gallup https://news.gallup.com/poll/200057/americans-rate-healthcare-providers-high-honesty-ethics.aspx
2. Phillips, N. (2017). Berry & Kohn’s Operating Room Technique. 13th Ed. St Louis: Elsevier.
3. Connor, R. Ed. (2018). Guidelines for Perioperative Practice. Denver CO: Association of PeriOperative Nurses.
4. AORN (2019). Guidelines for Perioperative Practice, Retrieved fromhttps://www.aorn.org/
