Aside from knowing essential lab value ranges, a nurse has to have a solid idea how to interpret those values, even though nurses don't diagnose or prescribe. In this article, we will discuss the complete blood count (CBC) and interpretation of the red blood cell-related values specifically.

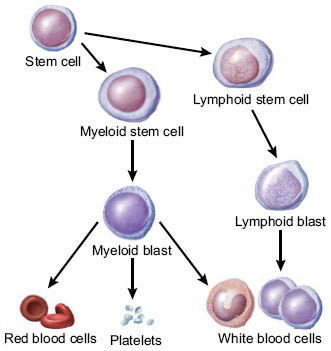
Think of how a baby grows into a person who will begin to function in a role in society - hematopoiesis is a similar idea. Stem cells grow and differentiate inside the bone marrow until mature enough to be released and do work in the body.
{This is a useful mental image to discuss when trying to explain leukemia to a client. What happens when the daycare is full of babies and there aren't enough mature adults? / What happens when the blood if full of baby blood cells instead of mature red cells, white cells, and platelets? The answer: All bad things! Chaos and so much more.}
This is one of many generalizations we will make here in order to simplify the understanding of the CBC! What these values mean for your client will vary on an individual basis.
CBC
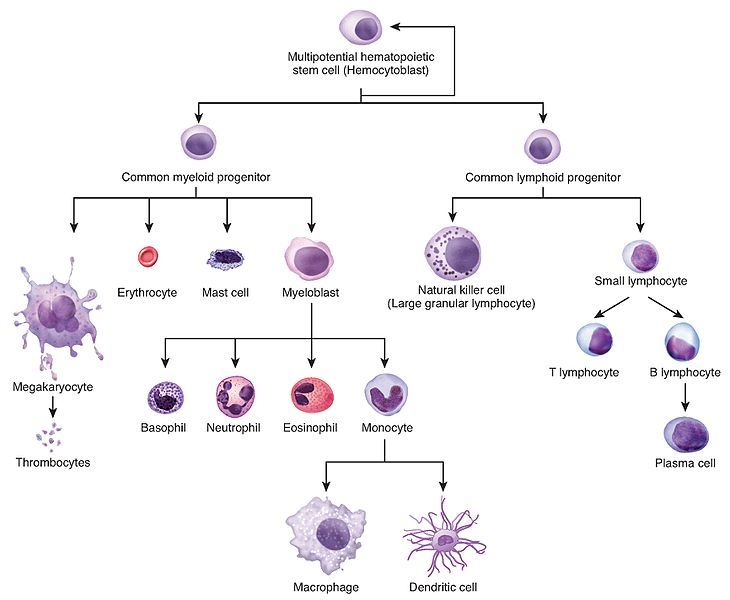
Where do baby blood cells come from? Hematopoiesis begins with stem cells in the bone marrow. These stem cells are baby cells that grow up to do specific jobs by becoming (1) red blood cells, (2) white blood cells, and (3) platelets.
A complete blood count is a test to determine how these mature, grown-up cells (RBCs, WBCs, platelets) are working, basically. Plasma, or serum, is the "blood" that is drawn for this test. Plasma is a mix of water, nutrients, antibodies, clotting factors, hormones, and many other key indicators of health and body function.
THE BASICS
Platelet count: Are there enough platelets to ensure effective clotting occurs in response to injuries? Is the platelet count too high and worrisome for causing unnecessary clots?
WBC count- Are there enough white blood cells to fight infection? Too many signaling there is an infection?
RBC count- Are there enough red blood cells to carry oxygen? Too many, blocking oxygen delivery to tissues?
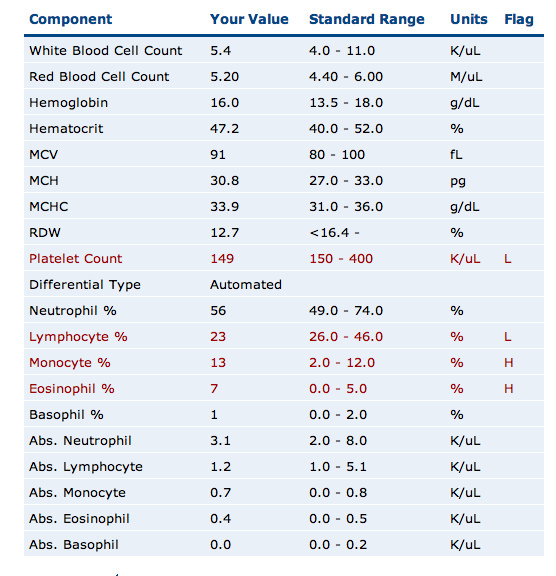
Platelet (Thrombocytes) Count
tells a story about the client's clotting abilities.
Platelets are only one way in which the body clots. When platelets are low, the client is at increased risk for bleeding. When platelets are high, the client is at risk for clotting. This, however, is only one part of the story. Looking at the platelet count is important for the nurse to determine if the client can go for an invasive procedure or needs an anticoagulant, for example.
Coagulation, the process of turning the blood into a semi-solid or solid - creating a clot, occurs through much more than just platelets. Activation of the coagulation cascade (or inhibition of coagulation!) includes coagulation factors. Platelet disorders, thrombosis disorders, procoagulants, anticoagulants, and the coagulation laboratory panel (INR, PTT - those things!) are a topic to be covered in another blog article!
White blood cell (Leukocytes) Differential
tells a story about what type of immune problem is occurring.
Ordered as a "CBC w/diff", the differential is essential in examining the components of the white blood cell and immune system. This is used in determining whether an infection is bacterial, parasitic, etc. A differential is a critical component of monitoring chemotherapy safety and leukemia or lymphoma progress.
Neutrophil count- These are essential to the initial fight against ANY infection. They are first responders to immune invader issues. High neutrophils indicate a bacterial infection, stress, inflammation, or injury. If someone has a low absolute neutrophil count (ANC), neutropenia increases risk for infections from usual and unusual sources. This number is SUPER important!
Monocytes- (Macrophages) eat dead cells and microorganisms. Monocyte percentages increase in response to parasitic, viral, and bacterial infections. Lymphocytes- B-cells create antibody-based immunity and increase in the presence of bacteria and viruses such as hepatitis, mononucleosis, or in blood malignancies; T-cells kills infected cells and cancer cells and are decreased in acquired-immune deficiency syndrome. Eosinophils- control inflammation and are high during parasitic infections and allergic reactions. Basophils- are elevated during asthma attacks and allergic reactions.These counts are less accurate if the client is taking steroids or other immunosuppressants.
The immune system is infinitely complex, and this is only a glimpse. There is much more to discuss when it comes to immune system function and dysfunction. This information is enough for the nurse to consider whether the client needs an anti-infective or needs to be protected from others who might be sick.
Red blood cell (Erythrocyte) Indices
tell a story about the kind of red blood cell anemia problem that is occurring.
Hematocrit- Is the percentage of RBCs correct for the amount of fluid in the body?
Volume expansion, such as occurs in pregnancy, results in a low hematocrit because there is more volume, reducing the percentage of red blood cell per volume of blood.
Volume depletion, such as occurs in the post-burn period or in dehydration from any cause, results in an elevated hematocrit because hematocrit is a percentage per volume of blood.
Hemoglobin- Is the protein content correct to carry enough oxygen to the body's tissues?
Athletes and high altitude dwellers tend to produce more erythropoietin due to tissue hypoxia, triggering increased hemoglobin. This enhances oxygen delivery to the tissues.
Smoking causes increased exposure to carbon monoxide, altering the ability of hemoglobin to carry oxygen. The body increases hemoglobin production to improve tissue oxygenation.

Indices reflect cell size and hemoglobin content.
MCV- The size of the red blood cell. Is the red blood cell larger or smaller than normal? Smaller cells can indicate fast bleeding and larger cells can indicate a slow bleeding source.
The average life span of an RBC is 1 1/2 - 2 months. If bleeding has occurred quickly (like might happen with an acute gastric ulcer), the body responds by making blood cells as quickly as possible, much more quickly than that 2 month life span of the RBC. Creating more RBCs to do the work needed. Microcytic anemia also occurs in response to decreased iron levels. Normocytic anemia occurs with very sudden blood loss or long term diseases, sometimes termed anemia of chronic disease. If bleeding has occurred slowly (like in colon cancer), the RBC become larger to increase the work each RBC can do. Macrocytic anemia occurs in response to chemotherapy or low B-vitamin levels. Poorly controlled diabetes causes swollen cells-a high MCV.
MCH- The count of hemoglobin found for each RBC.
Low hemoglobin per cell counts occurs due to iron deficiencies- Hypochromic anemia. One way this happens is through very frequent blood donations which depletes the liver's iron stores. Normochromic anemia occurs with very sudden blood loss or long term diseases, sometimes termed anemia of chronic disease. High hemoglobin per cell counts are often the result of the same things that cause macrocytic anemia - Hyperchromic anemia. Extra iron attaches to each red blood cell to compensate for this type of anemia. B12 deficiency results in high MCV and high MCH.
MCHC- The amount of hemoglobin compared to the size and volume of the RBC. This value has limited usefulness alone, but is used in conjunction with other lab values.
RDW- The variation in red blood cell circumference or width. High RDW and high MCV might indicate a nutrient deficiency (iron, B12). If RDW and MCV are normal, but the client is anemic, this might indicate anemia of chronic disease.
If red blood cell indices are indicated to diagnose a client, a peripheral blood smear performed by qualified lab personnel, is also indicated.
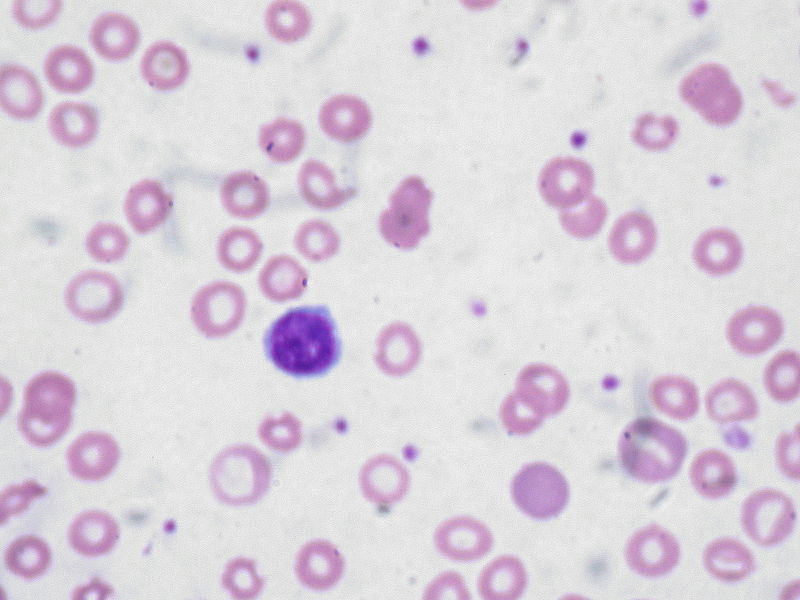
ANEMIA
Erythrocyte indices help determine where to look next to determine and correct the problem. Though an individual can have increased red blood cells (polycythemia), there are many, MANY causes of decreased red blood cells.
Anemia has 3 basic causes: (1) The body doesn't make enough RBCs (2) There is too much bleeding (3) The body destroys RBCs.
(1) The body doesn't make enough RBCs.
- Not enough iron to make hemoglobin for red cells.
- Not enough folate or vitamin B-12 to produce red cells.
- Not able to process B-12 (pernicious anemia).
- Anemia of chronic disease is an inflammatory process that inhibits the production of RBCs.
- Aplastic anemia from infection, medication, autoimmune disease, or toxic exposures.
- Leukemias and other bone marrow diseases that interfere with stem cell production and maturation.
- Alcohol abuse is toxic to hematopoiesis and reduces production.
(2) There is too much bleeding (large hematoma).
Chronic bleeding or Acute bleeding
- Lung or colon cancer, gastric ulcer, trauma, post-surgical hematoma, postpartum hemorrhage, excessive anti-coagulation, thrombocytopenia, hemorrhoids, varices.
- Many other causes can cause slow bleeding or rapid blood loss. Blood loss can begin slowly and become rapid, too!
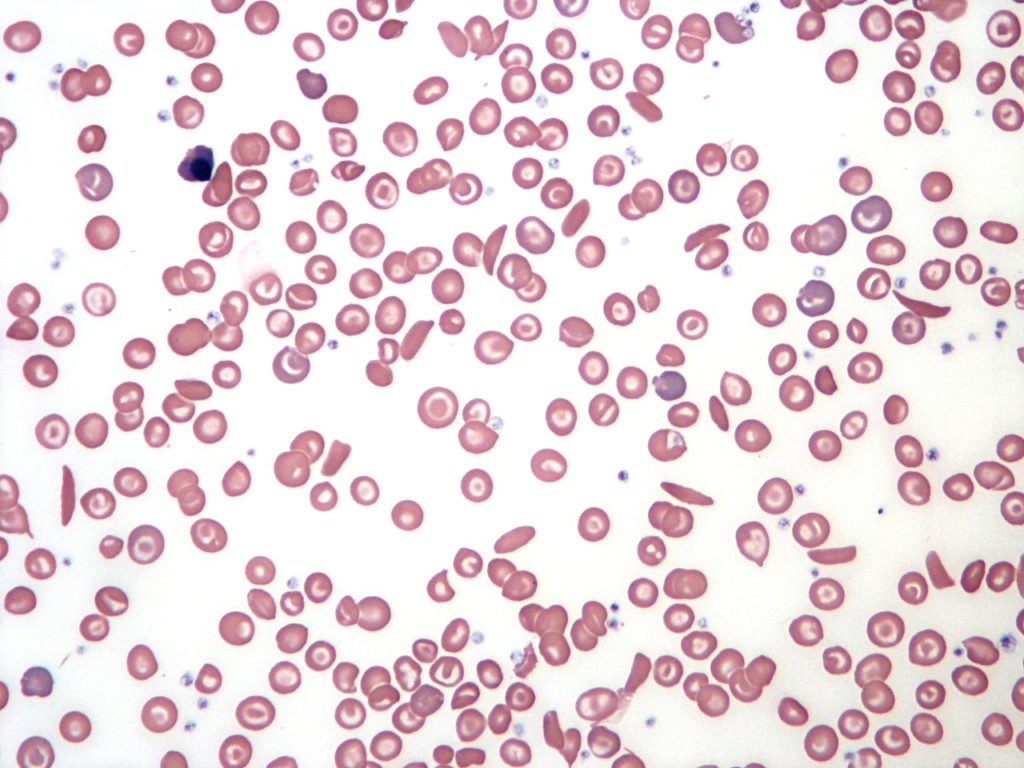
(3) The body destroys RBCs.
- An enlarged spleen secondary to cirrhosis, mononucleosis, malaria, or chronic lymphocytic leukemia.
- Hemolytic anemia secondary to prosthetic heart valves.
- Disseminated intravascular coagulation (DIC).
- Incompatible blood transfusion (hemolytic reaction).
- Sickle-cell anemia causes the crescent-shaped red cells to be destroyed prematurely.
Of course, the best treatment for anemia is treating the cause, and we've only listed a very few of those causes here!
How to treat the causes of anemias is a topic for another day, though!

CHECK US OUT!
Join our fabulous nursing community @ https://www.facebook.com/NursingandNCLEXMastery/
Blog article sources:
http://www.hematology.org/Pati...
https://medlineplus.gov/ency/a...
https://www.ncbi.nlm.nih.gov/b...
https://www.mayoclinic.org/dis...
https://www.mayoclinic.org/dis...
https://www.mayoclinic.org/dis...
https://emedicine.medscape.com...
https://www.healthline.com/hea...
https://emedicine.medscape.com...
Image sources:


Flickr image of CBC results- link embedded



https://commons.wikimedia.org/...">">
.jpg)
https://commons.wikimedia.org/...




